Atrial fibrillation is a very common cardiac issue, although I am hearing about more and more people being diagnosed with it, and I am getting lots of questions from readers about this diagnosis. Again, it is very common, and I think that people should be aware of the symptoms, the causes, and the treatment of this cardiac arrhythmia (and arrhythmia is just when the heart beats at an abnormal rate or rhythm.)
 What is Atrial Fibrillation?
What is Atrial Fibrillation?
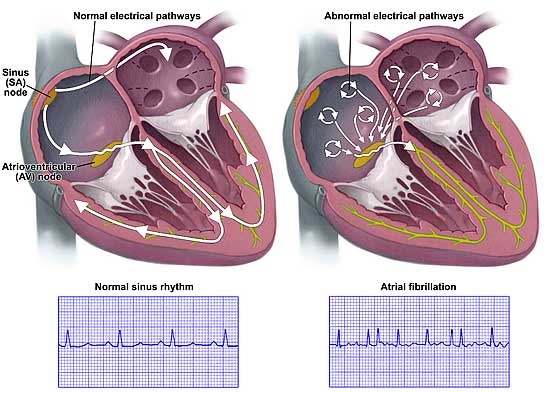
It is an abnormal heartbeat, that can be very rapid, and lead to poor blood flow to various parts of the body, as the heart isn’t able to completely fill with blood before contracting (each beat), so only some of the blood that should be going out through your arteries to the extremities is available. The atria (the top two portions of the heart) are beating faster and not in sync with the ventricles (the lower portions of the heart.) Normally the Sinus Node (a group of cells in your heart) act as a natural pacemaker for you heart; it sends out a signal that passed through the atria (the upper two chambers of your heart) and causes them to contract and pump blood into the ventricles (the lower to chambers), then the signal hits the AV (atrioventricular) Node, which causes the ventricles to contract and move blood out from the heart into the extremities. in Atrial Fibrillation, the Sinus Node sends chaotic signals, so the atria are quivering in attempting to respond to each electrical signal, and the AV Node becomes overwhelmed with the electrical signals as well, so the ventricles also beat faster than normal (though not as fast as the atria). The normal heart rate is 50-90 and in AFib your heart rate can be as fast as 100-175 beats per minute.
It is normally not life threatening, as people live with it chronically, or they flip in and out of it, but it can have some serious complications, and if you go into a rapid a fib, you should be seen immediately by medical services, especially if you are feeling unwell, light-headed, etc. There are various different treatments, including medications and electrical treatments. Many people live long lives with chronic atrial fibrillation, it is just important to know the symptoms, treatments, risks of treatments, and when you should seek immediate medical attention.
What are the Symptoms?
*If you have any of these symptoms, you should be seen by your HCP to get your heart checked out and make sure that is the source. Also, as I said above, there is paroxysmal AFib which comes and goes with symptoms, and chronic, in which your heart is continuously in this abnormal rhythm.
-Palpitations (a fluttering in the chest, rapid/racing heart rate)
-Weakness
-Lightheadedness
-Confusion
-Shortness of breath
*If you ever have chest pain along with any of these symptoms, or alone, you should seek immediate medical attention because you may be having a heart attack. Please go to the nearest emergency department or call 911.
What are the causes of AFib?
-Congenital heart defects (heart defects you are born with)
-Heart Attacks
-High Blood Pressure
-Heavy use of stimulants (caffeine, medications, tobacco)
-Heavy alcohol use
-Sick Sinus Syndrome (a defect of the sinus node where it speeds up on its own)
-Emphysema or other chronic lung diseases (like Chronic Obstructive Pulmonary Disease COPD)
-Abnormal heart valves
-Prior cardiac surgery
-Viral infections
-Sleep Apnea (where you lose your airway for short periods of time while sleeping)
-Stress from Pneumonia or other illnesses
What will put me at higher risk?
-A family history: If anyone in your family, especially a close relative has AFib, you are also at risk.
-Age: The older you are, the more increased your risk becomes. Especially if you have any chronic illnesses
-High Blood Pressure: If you have uncontrolled high blood pressure, you are at a higher risk for AFib. If you have made the proper lifestyle changes to get more exercise, eat healthy, and take medications to treat the blood pressure, then your risk shouldn’t be increased.
-Heart disease: If you have a history of heart attacks, valvular disease, heart surgery, or other arrythmias.
-Drink Alcohol: Usually binge drinking (5 drinks in two hours) can put both men and women at a higher risk for atrial fibrillation. (take heed college students!)
What are the major Complications?
Well, one of the biggest risks is stroke. When the atria are quivering and not completely expelling all of the blood they fill with to the ventricles, the blood leftover is at risk to clot (little micro clots) and when they get ejected eventually into the blood stream, it can travel to the brain, impede blood flow, and cause a stroke (death of some of the brain cells due to a lack of blood flow.) Also, when your heart is working so hard constantly, without treatment, it can lead to heart failure; your heart is unable to meet the demand of your body by being able to eject enough blood to get to where it needs to go.
How is AFib diagnosed?
It is early important to bring with you a list of symptoms of your HCP, when you most experience them, all of your past medical history, any and all medications you take, and be very honest with your HCP about your lifestyle (eating habits, exercise, etc.) Your HCP will take that into account when doing your physical assessment, listening to your heart sounds, and checking your blood pressure and heart rate. You will also most likely have:
–An EKG: an Electrocardiogram which is a 12 lead assessment of the electrical impulses of your heart. 12 little stickers are placed on the skin on your chest, and little plastic/metal leads are connected, you will be asked to stay still for about 30 seconds, then a print out of your hearts impulses comes out. It shows what is going on and is not very invasive at all, and a snap shot of your heart.
–A Holter Monitor: A monitor with about 5 leads is attached to your for 1 to 2 days, and is worn under your clothing, it constantly checks the rhythm of your heart and if you feel symptoms, you push a button, and all of that information is downloaded by your HCP so they can correlate symptoms and your heart rhythm.
–An Event Recorder: Similar to a Holter monitor, but worn for a month, and it only records when you have an arrhythmia, and it sends signals to your HCP when you have those events, and it helpful at showing when arrhythmias happen at unexpected times (like during sleep.)
–Echocardiogram: basically an ultrasound of your heart through your chest wall, there is some lubricant applied to your chest, and a hard plastic wand is moved over it to show how your heart is functioning and can give a 3D view of the actual functioning of the heart. It can help to diagnose if you have any structural abnormalities.
–Blood Tests: your HCP will check to see if you have a thyroid problem or any other electrolyte abnormalities that would cause your heart to beat irregularly.
–Chest X-Ray: Just a quick and less invasive way to see your heart and lungs and diagnose a possible pneumonia that could cause your symptoms.
What are the treatments?
The treatments are aimed at controlling your heart rate and preventing blood clots. If you are caught quickly with the arrhythmia, you can be cardioverted (your heart rate can be attempted to be manipulated and changed) back to a normal rhythm using either electricity (you will be given sedation and get a moderate amount of electricity to shock the heart back into a normal rate) or you can be given Intravenous medications to do the same thing (which requires monitoring and a possible overnight in the hospital). Before any form of cardioversion you will be given a blood thinner to prevent clots from forming and from being ejected into the blood to prevent a stroke. And you will also have to take the medications for 4-6 weeks after a successful cardioversion. Most often Coumadin (warfarin) is used as a blood thinner, but you have to be careful, as there are MANY side effects with Coumadin (and the other blood thinners commonly used such as Dabigatrand and Rivaroxaban.)
If the cardioversion is NOT successful, you will be kept on a blood thinner and a medication to keep your heart rate 60-90 and prevent the rapid Atrial Fibrillation. Some of the medications that may be used to rate control your heart are:
-Amiodarone (Cordarone)
-Dofetilide (Tikosyn)
-Metoprolol (Lopressor)
-Sotalol (Betapace)
-Dronedarone (Maltaq)
There are two surgical procedures that can be done that can treat AFib as well. A radio ablation is when the HCP puts a catheter through your groin artery into your heart, and where there are areas of “hot spots” or cells that are acting like a pacemaker (like your Sinus Node), electricity is used to ill off those hot spots and cause scarring. Electrical impulses in the heart cannot go through scar tissue. There is also a surgical Maze procedure where there are small cuts made in the heart tissue to also cause scaring and prevent the electrical impulses from causing the quivering of the atria; this needs to be done during open heart surgery so is usually down when someone is having open heart for another reason (such as valvular repair) and if they do not respond to other treatments. These are both pretty invasive, but if you do not want to chronically be on medications or are not responsive to medications, they are great options.
How do I prevent AFib?
Some of the risks you have no control over, like family history or congenital defects, but overall, living a healthy lifestyle, eating low-fat and low sodium, and getting at least 20-30 minutes of exercise daily greatly helps you in preventing AFib. Also, quit smoking, and don’t intake too many stimulants (maybe you don’t need that 4th cup of coffee and lay off the 5 hour energy?). Try to limit your drink in g to 1-2 drinks per day, and just be aware of the symptoms. If you are at all worried about your risks, or you have any of the symptoms, talk to your HCP and see if there is anything else you can do to prevent AFib.
Yours In Good Health
B